Early Q1 Engagement of New Members Drives 2-5% Higher Plan Retention
By Sai Balusu
Executive Summary
New ACA and Medicare Advantage members who receive personalized, proactive outreach and complete preventive visits in Q1 show a 2–5% higher retention rate by the end of their first plan year, according to N1 Health’s findings across multiple health plans. For every 10k new members, this retention lift translates up to $6m of retained revenue and up to $1m of margin.
This insight matters because health plans often wait until mid-year to engage new members in completing a preventive visit, missing a critical early window when behavior and trust are easiest to influence. Building member trust with early coordinated engagement directly influences CAHPS, Stars, and long-term medical cost trends.
This article outlines what health plans should do to provide new members a best-in-class experience to increase retention, and how N1’s consumer data and predictive models can enable this through personalized, high-impact engagement at scale.
Key Insight: Early Q1 Engagement for New Members is a Critical Retention Lever
Q1 is uniquely powerful. Across multiple health plans and markets, new members who complete a preventive visit in Q1 show 2% to 5% higher retention compared to those who engage later or not at all.1
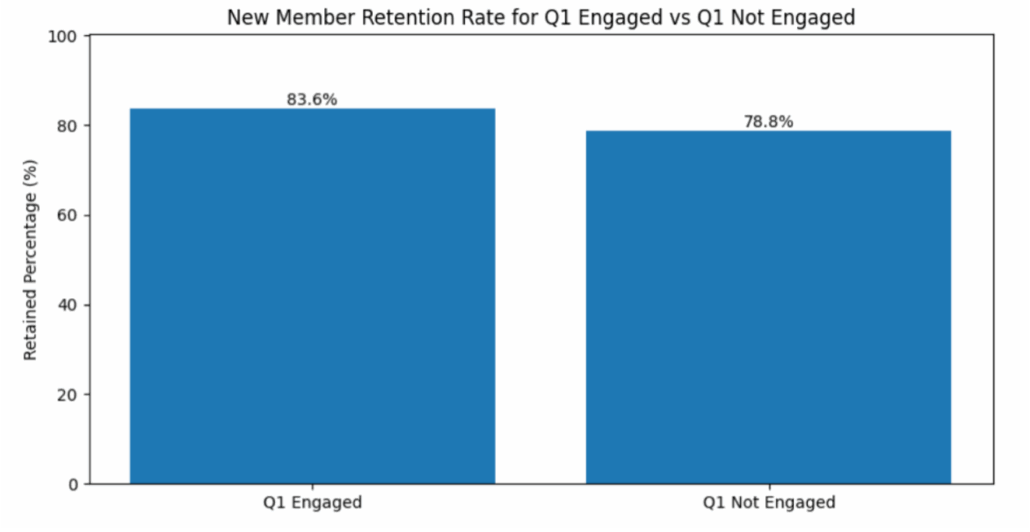
1 Please find detailed description of statistical methodology and outputs of analysis below.
During Q1, members are forming impressions, resetting healthcare habits, and deciding whether the plan experience feels simple or frustrating. We’ve all been there, right? Historically, outreach campaigns start in Q3–Q4 which is much too late to influence trust, utilization, or satisfaction for the plan year. The cost of inaction in Q1 is increased avoidable medical cost, decreased member retention, and worse quality ratings.
Early engagement isn’t just “nice to have”, it directly drives measurable outcomes. For every 10k new members, this retention lift translates up to approximately $6m in retained revenue and up to $1m in margin – before accounting for additional downstream savings related to avoiding preventable medical events, increased quality gap closure, and improved Star ratings.
Personalized, proactive engagement matters. Identifying new members’ specific needs, addressing barriers to care, and delivering coordinated, personalized communications are key strategies to boost preventive visit rates and reduce disenrollment and dissatisfaction.
What Health Plans Should Do Next
To provide a differentiated new member experience and stay competitive in the market, health plans need to run a proactive campaign in Q1 targeting new members early with personalized messaging aligned to their specific needs, encouraging them to schedule a preventive visit, and help them overcome any hurdles they face in their care journey.
- Use predictive models to identify who is least likely to engage on their own — and what channels/times are optimal.
- Remove barriers by providing quick PCP/AWV appointment scheduling links, PCP selection support, In Home Assessment options, and benefit education tailored to each member.
- Monitor engagement in real time and adjust frequency, messaging, outreach channels, and time of day based on lift.
This creates a high-trust first experience and increases the likelihood of long-term plan engagement.
How N1’s Technology and Services Make This Possible
The biggest challenge most health plans face is not knowing enough about these members because they are new to the plan and therefore lack any historical data. This prevents health plans from creating tailored messages and delivering a positive, unique, member-centric experience. Instead, health plans blast one-size-fits-all onboarding messages to all their new members, increasing member abrasion and eroding member trust.
This first engagement is uniquely powerful to create a successful long-term relationship with the member and earn durable member trust. N1 helps health plans maximize the impact of this first engagement by using predictive models and individual-level consumer data to pinpoint which new members need early engagement and what unique message will resonate the most for each member.
We operationalize the entire workflow—identifying members, prioritizing outreach, creating personalized messages, and orchestrating channels. This makes proactive Q1 new member engagement personalized, scalable, measurable, and outcome driven.
Health plans using our approach consistently see higher AWV completion, stronger member retention, and lower avoidable cost in members’ first year on the plan. For example, a national ACA plan using N1’s data and models to personalize their new member experience, saw a 46% increase in new member AWV completion rate, and a 3% increase in retention rate compared to the established control group.
Q1 is the time to act! If you are interested in understanding the retention, Stars, and financial upside for your New Member population, our team can run a cohort analysis and build a ready-to-execute Q1 New Member Engagement plan. Reach out to our team to see how predictive, personalized new-member engagement can work for your plan in just a few weeks.
Proactive Q1 engagement applies not just to new members, but also to historically unengaged, and high-risk members. An upcoming article will highlight how N1 can help identify the right members (new, unengaged, and/or high risk) that need to be engaged early in the year with a tailored member engagement strategy to ensure members are retained long-term, reduce avoidable medical expenses and improve the overall member experience.
____________________________________________________________________________________________________________________________________________
Statistical Methodology
To quantify the true impact of early-year preventive engagement for new members, we aggregated and analyzed multi-year datasets from multiple health plans spanning different geographies and lines of business. The objective was to isolate the causal effect of new members completing a preventive visit in Q1 on downstream retention and experience outcomes.
To do this fairly, we used a technique called propensity score matching, which ensures we’re comparing apples to apples—not healthier, more engaged members against those who were already at higher risk. This method controls for factors like age, social risks, transportation difficulties, digital access, health literacy, household characteristics, income indicators, and more. After matching, all covariates were balanced within a 3–5% standardized difference, indicating strong comparability. Results were statistically significant (p < 0.001), meaning the observed retention lift is unlikely due to chance.
This reduces bias and ensures the difference in outcomes reflects the impact of engagement timing, not pre-existing differences in the populations. It gives us confidence that the 2%–5.5% lift in retention is truly driven by early engagement—not external factors. It’s a rigorous approach health plans can trust to represent a real, viable opportunity.