Early Q1 Preventive Visits Reduce Avoidable Costs by $640 PMPY and Improves Adherence by 14%
By Sai Balusu
Executive Summary
N1 Health’s multi-year, multi-market analysis of Medicare Advantage and ACA members shows that completing a preventive visit in Q1 leads to a $640 PMPY reduction in avoidable medical expenses and a 14% increase in medication-adherence rates compared to those who complete a visit later in the year. This represents an annual savings of $6.4M for every 10,000 members.
Health plans often wait until mid-year to engage these members and get them to complete a preventive visit, missing a critical early window when behavior and trust are easiest to influence. This often leads to Q4 sprints with members being bombarded by a large number of messages coming from all parts of the health plan organization.
This post outlines what health plans should do instead, and how N1’s consumer data and predictive models enable health plans to change their operational workflows and implement coordinated engagement campaigns early in Q1. This ensures that members receive care sooner and leads to increased visit completion rates, improved CAHPS and Star ratings, and reduced long-term medical costs.
Key Insight: Early Q1 Engagement Leads to Increased Cost of Care Savings
Across multiple health plans and lines of business, members who completed a preventive visit in Q1 had significantly improved outcomes vs similar members who completed the same visit later in the year — including a reduction in avoidable medical spend by $640, and a 14% increase in medication adherence. Our analysis defined preventive visit types as inclusive of general preventive visits, Annual Wellness Visits (AWVs), and Well Child Visits (WCVs).
Early engagement isn’t just “nice to have”, it directly drives measurable outcomes. For every 10,000 members that complete a visit early, a health plan stands to save $6.4M in medical costs annually.
Table 1: Clinical outcomes in members that completed a Q1 visit vs later in the year1
| Outcome Metric | Percent Decrease |
| ED Visits | 9-13% |
| ED Days | 13-21% |
| IP Visits | 17-40% |
| IP Days | 19-50% |
1 Please find detailed description of statistical methodology and outputs of analysis below.
Early Q1 engagement isn’t just clinically beneficial; it creates operational breathing room and sets the entire year up for success. Today, most members are inundated in Q3 and Q4 with overlapping outreach for AWVs, quality gap closure, medication adherence, and other initiatives. That concentrated surge of messages overwhelms members, creates confusion, and dilutes engagement.
By shifting preventive outreach into Q1, health plans can smooth operational demand across the year and build stronger habits with members earlier, before outreach fatigue sets in. Members who complete preventive visits in Q1 establish better care patterns, respond more consistently to future outreach, and face fewer downstream barriers to follow-through. In addition, with members receiving fewer overlapping messages later in the year, the remaining Q3–Q4 outreach becomes more effective and less abrasive, reducing member frustration while improving plan performance and retention.
What Health Plans Should Do Next
Health plans should treat January through March as the foundation-building period for member behavior. Early engagement isn’t just about closing one visit; it’s about helping members get the right support from day one by addressing their specific care barriers and building strong long-term habits for their care. This is especially critical for rising risk and historically unengaged members who benefit most from structured guidance about the healthcare services they can access earlier in the year.
The beginning of a new plan year often serves as a natural reset for members, prompting them to reprioritize health, revisit care decisions, and adjust routines. Combined with plan-related changes—such as PCP selection, benefit updates, or medication changes—this period can reveal engagement barriers like transportation limitations, caregiving demands, or gaps in digital access. By identifying these circumstances early, health plans can pair preventive visit scheduling with proactive, tailored support such as personalized supplemental benefit guidance (e.g., free transportation for medical appointments), mail-order pharmacy enrollment, and member education that improves medication understanding and care literacy. This early, personalized support builds trust, reduces abrasion, and sets members up for sustained success throughout the year.
Most health plans cannot — and should not — attempt to engage all members at once. Operational capacity, call-center bandwidth, care management, and provider scheduling constraints make blanket outreach impossible. Instead, health plans must use individual level data and predictive models to identify specific needs members have and prioritize the member outreach accordingly. Without this prioritization, outreach becomes diluted and ineffective.
How N1’s Technology and Services Make This Possible
Early-year engagement only works when health plans know which members to prioritize and what support each member needs. N1 makes that possible through three core capabilities:
- Predictive models that identify rising-risk and hard-to-reach members
- Our models analyze thousands of factors such as social risk, care patterns, utilization, gaps, adherence signals, chronic conditions, life transitions, and pinpoint members who are most likely to:
- Delay preventive (inclusive of preventive visits, AWV visits, PCP visits)
- Experience avoidable ED or inpatient events
- Become non-adherent and have open gaps in care
- Churn from the plan
- Our models analyze thousands of factors such as social risk, care patterns, utilization, gaps, adherence signals, chronic conditions, life transitions, and pinpoint members who are most likely to:
- Member-level data that uncovers each person’s unique needs
- We leverage hundreds of data elements per member on life events, behavioral indicators, and household characteristics, that reveal what barriers members are facing right now, including:
- Recent moves or PCP changes
- Digital divide indicators
- Transportation constraints
- New medications and care transitions
- Health literacy challenges
- Caregiver or household burden
- We leverage hundreds of data elements per member on life events, behavioral indicators, and household characteristics, that reveal what barriers members are facing right now, including:
- Personalized outreach workflows that scale
- Our Customer Success and Data Science team convert these model outputs and member insights into tailored outreach strategies that meet members where they are:
- Outreach that adjusts to the member’s risk, preferences, and barriers
- Recommended timing and channel mix for each member
- Content templates that speak to the member’s real situation
- Our Customer Success and Data Science team convert these model outputs and member insights into tailored outreach strategies that meet members where they are:
These capabilities allow Health Plans to operationalize Q1 outreach at scale; not by contacting everyone, but by prioritizing and focusing on those members who need it the most and will drive measurable improvements in retention, cost of care, and Star ratings.
N1 brings the expertise of designing and running these programs across the industry for nearly a decade. We bring the best practices in intervening early, supporting members from day one, building long-term care habits, and meaningfully impacting member outcomes. By aligning predictive intelligence with personalized engagement, our product enables a proactive Q1 strategy that consistently improves retention, adherence, CAHPS, and lowers avoidable medical expense.
If you want to understand which members to prioritize in Q1, and how much financial value is at stake, we can run this analysis on your population within days. Let’s talk about building your Q1 engagement plan!
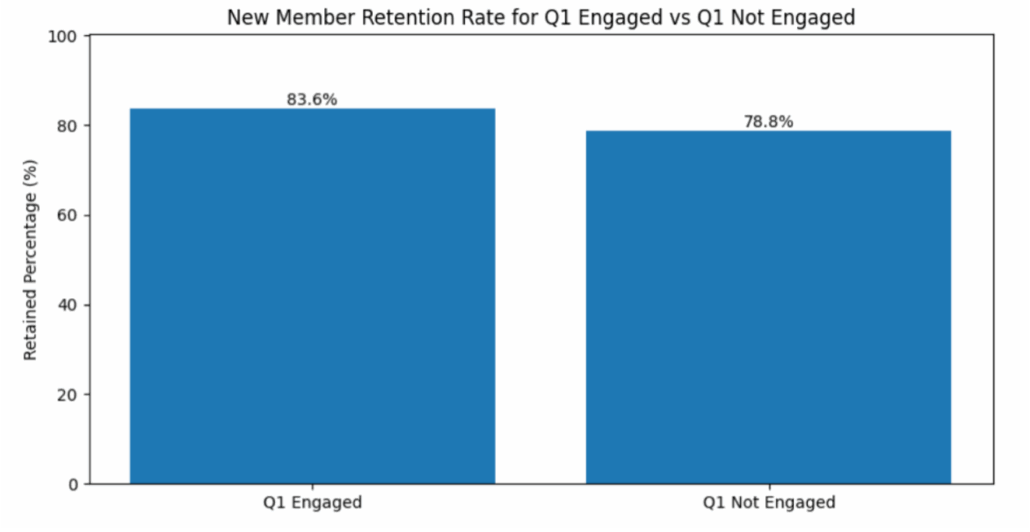
Proactive Q1 engagement applies to both high-risk members, and new members. Check out this article to understand how the right New Member Engagement strategy can lead to 2-5% increased retention. In addition, an upcoming article will highlight how N1 can combine both strategies to identify the right members that need to be engaged early in the year and ensure a tailored member engagement strategy that leads to long-term member retention, reduction in avoidable medical expenses, and improvement in the overall member experience.
____________________________________________________________________________________________________________________________________________
Statistical Methodology
To quantify the true impact of early-year preventive visit engagement for members, we aggregated and analyzed multi-year datasets from multiple health plans spanning different geographies and lines of business. The objective was to isolate the causal effect of members completing a preventive visit in Q1 on downstream cost of care and quality outcomes.
To do this fairly, we used a technique called propensity score matching, which ensures we’re comparing apples to apples—not healthier, more engaged members against those who were already at higher risk. This method controls for factors like age, chronic conditions, past utilization, social risks, transportation difficulties, digital access, health literacy, household characteristics, income indicators, and more. After matching, all covariates were balanced within a 3–5% standardized difference, indicating strong comparability. The results were statistically significant (p < 0.001), meaning the observed retention lift is unlikely due to chance.
This reduces bias and ensures the difference in outcomes reflects the impact of engagement timing, not pre-existing differences in the populations. It gives us confidence that the $640 annual reduction in avoidable medical expenses, and the 14% increase in medication-adherence rates are truly driven by early engagement and not external factors. It’s a rigorous approach health plans can trust to represent a real, viable opportunity.